The watchman procedure is becoming popular among stroke patients looking for an alternative to drug treatment therapy. It has been implanted in over 10,000 patients worldwide—and the results have been fantastic. Surgical treatment is painless and quick, with a 94.7% success rate. If you consider the procedure, it is important to talk with your doctor about the pros and cons of watchman device. Let's dive into the details and find out.
A watchman device is a medical device placed in the chest to help prevent clotting in people at risk for stroke. The device is also known as a left atrial appendage closure (LAAC) device. The watchman device is placed in the heart through a catheter, a thin tube inserted through a vein in the leg. Once the device is in place, it permanently blocks off the left atrial appendage (LAA) opening, a small pouch attached to the heart's left atrium. The LAA is where most strokes related to atrial fibrillation occur.
Atrial fibrillation is an irregular heartbeat that can cause blood to pool in the heart and form clots. If a clot breaks free and travels to the brain, it can cause a stroke. The watchman device is designed to reduce the risk of stroke by preventing clots from forming in the LAA.
There are many possible pros of watchman device in case of atrial fibrillation. Here are some of the practical benefits of the watchman procedure.
One of the biggest advantages of the watchman device is that it can significantly reduce your risk of stroke-related atrial fibrillation. The device effectively prevents blood clots from forming in the LAA, reducing the likelihood that a clot will break free and travel to the brain.
It may allow you to avoid or reduce your dependence on medications such as warfarin (Coumadin) or other blood thinners. Many people with atrial fibrillation must take one or more blood thinners daily to help prevent clotting in their heart, but these drugs can be expensive and often cause side effects such as bruising or bleeding. One of the prominent pros of watchman device is that you don't require daily medication.
In addition to reducing the risk of stroke, the watchman device also reduces the risk of bleeding or other complications associated with blood thinners. These medications are commonly used to prevent clotting in atrial fibrillation patients; they can sometimes cause adverse effects such as bleeding or internal bleeding. By eliminating the need for blood thinners after placement of the watchman device, many people experience improved overall health and quality of life compared to those who continue taking blood thinners.
The watchman device can also improve the quality of life for many people with atrial fibrillation. The device can help prevent strokes, often leading to disability or even death. Additionally, the watchman device can help reduce the need for blood thinners, which can often cause side effects that impact a person's quality of life.
Although there are several potential advantages, there are also some cons of watchman device. These include the risks associated with the procedure itself and the potential for the device to fail over time.
One of the main cons of watchman device is that it involves a minimally invasive procedure to implant the device in the LAA. This procedure carries some risk of complications, including bleeding or infection.
In addition to these risks, there is also a chance that the watchman device may fail over time. As with any medical device, there is always the possibility of failure due to manufacturing defects or other issues. While this risk is relatively low overall, it can be a significant concern for some people and should be carefully considered before using this type of device.
Another drawback of watchman device is that it is not widely available. This device is currently only approved for use in the United States, and it is not clear when or if it will be available in other countries. Additionally, all insurance plans do not cover this device, so patients may have to pay out of pocket for the procedure.
The device requires regular monitoring. Patients who have this device implanted will need to visit their doctor regularly to ensure that the device is functioning properly and they are not at risk for complications.
Conclusion on the Pros and Cons of Watchman Device
After understanding the pros and cons of watchman device, you can consult your doctor to help you decide whether it's a go-to option for you or not. The pro list is impressive, but it's important to weigh all the factors involved in such an important decision. And be sure to stay up-to-date on the latest news and research about this cutting-edge technology.
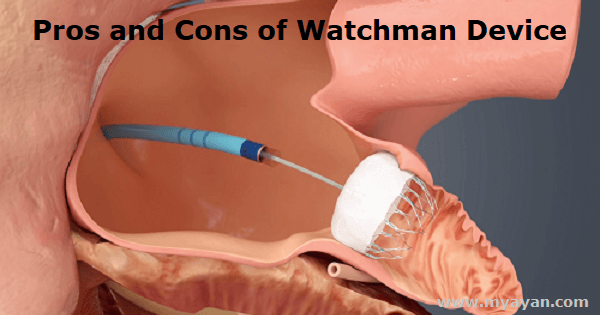
The good news is that a new FDA-approved gadget called the WATCHMAN can be used as a long-term treatment for those with atrial fibrillation or an increased danger of stroke. The even better news is that the WATCHMAN procedure has shown to be successful in 94.7 percent of patients, according to studies.
The LAA is accessed through a small incision in the upper leg, accompanied by the placement of a narrow tube. The Watchman is a minimally invasive, permanent, one-time surgery that takes less than an hour to complete.
According to Boersma et al., the Watchman implantation was successful in 98.5% of cases, with no residual flow in 99.8%.
Despite late-stage extraction with full endothelialization, most devices may be removed safely, allowing high-risk patients an alternative therapy to lifelong anticoagulation.